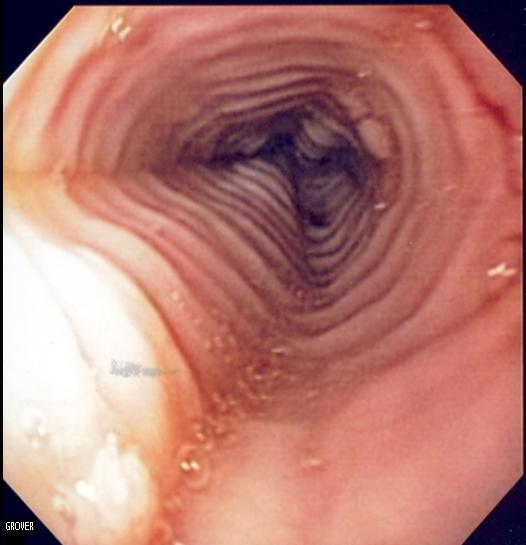
Eosinophilic Esophagitis and Celiac Disease EP069
Your gastrointestinal tract is approximately 30 feet long, and it runs from your mouth all the way to the anus! We know that celiac disease can impact any part of the digestive tract. But there is another disease that wreaks havoc on the GI tract as well, a condition called eosinophilic esophagitis or EoE. The […]
Eosinophilic Esophagitis and Celiac Disease EP069 Read More »